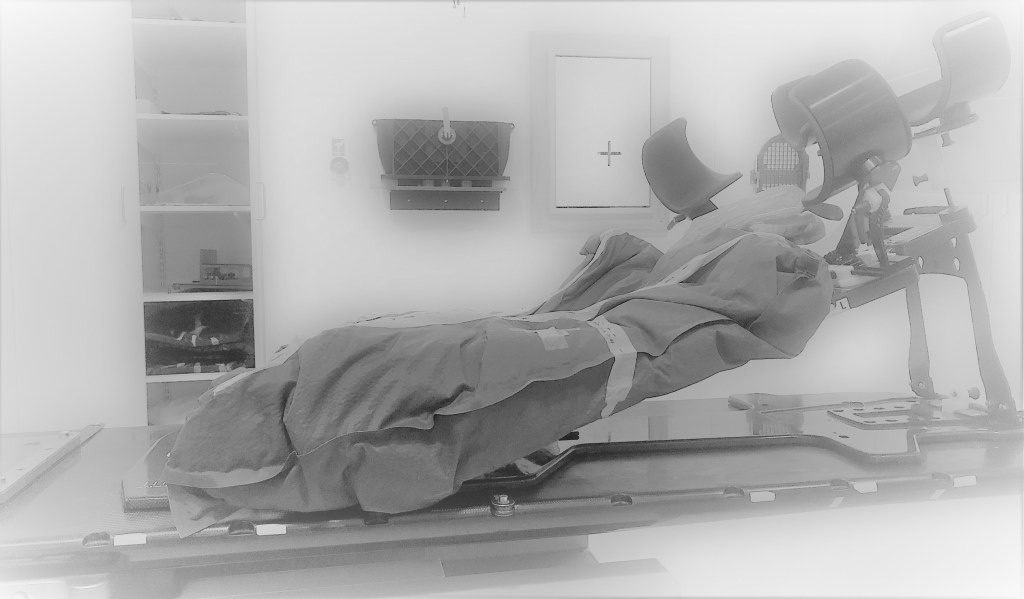
Alt text: An edited black & white image of a hospital room containing radiotherapy equipment – the table, arm cuffs & a special piece of equipment – similar to a weatherproof sailing bag, moulded to my shape – which held me in position for the treatment.
Beam me up:
6 weeks after having breast cancer surgery (a lumpectomy), I received 5 days of partial radiotherapy. Apparently, the success rate of this treatment is quite high & its use is on the increase. I was glad to have this option because, 9 months later, there is no evidence that this treatment has adversely affected my lungs.
The most difficult aspect of the radiotherapy for me was coping with the equipment. Before embarking upon the treatment, the breast cancer team did a couple of checks – one was whether I could raise both arms easily (I could) & the other was whether I could get on & off the treatment table independently. This was slightly trickier, but because I use my right leg to do quick standing transfers in & out of my wheelchair, I managed it in quick time (it surprises people when wheelchair users can stand & do a quick transfer. I know not every wheelchair user can do this, but I’m always amused by people’s reactions at my speedy manoeuvres in & out of my chair).
However, when I went for my preparation & assessment day, I discovered that the radiotherapy table is far higher that the consultation table & it doesn’t really move up & down. For scale, I’m a little over 1m tall so the table was the same level as my head! When I first saw the table, I exclaimed: “Blimey, I wasn’t expecting it to be this high, I’m not sure I’m going to manage this!” The whole set-up looked really foreboding. The equipment honestly looked like it belonged in some kind of sex dungeon. For the radiation beams to be aimed, you need to be topless, so once I’d placed my arms above my head into the cuffs, I felt really exposed, submissive & vulnerable. (I bet a man designed this equipment – no woman would ever design something that leaves patients in an undignified position!) One of the nurses expressed that the equipment should be painted pink so that it would be more appealing. I replied with “yeah, may-be” but apart from the gender-stereotyping issue, I’m not sure any colour would improve its “torture chamber” look.
A large step was brought into the room, so I clambered onto that & after 3 failed attempts, I managed to heave myself up on the table, supported by my Personal Assistant & two team members. So bloody painful 6 weeks after surgery to my breast & armpit!
The next hurdle was making sure that I didn’t slip down & off the table. This really wasn’t easy. The surface of it is metal & the table itself is actually very narrow. Not only was I sliding down it, but I was also sliding off it because of my wonky balance! To stop patients sliding, there is a metal bar drilled into the table (you can just see it to the left-hand side of the image), but my legs are different lengths & my left foot is paralysed so I have no grip. I tried to grip the sides of the table, but then the radiotherapy team told me that I had to raise my arms & fix them into cuffs, so that they could administer the treatment to my chest & ribs. Because of the nature of the treatment, there is little room for adjustment to the equipment.
We all had to improvise on the spot of how to get around this issue. I had to get off the table again which involved pivoting & slowly lowering myself down onto the step (my poor arm!) Then one of the team said that with some patients, they use what I can only describe as a “suction bag” – you’re settled into the bag on the table & placed in position for the treatment. Then all the air is suctioned out of the bag which moulds it to your shape & enables you to stay in position. You can see the bag & how it’s mould to my shape in the image – it’s similar to a weatherproof sailing bag. It really is such a clever device & without it, I couldn’t have gone ahead with the treatment. The bag was marked up with my name & each time I had treatment, my bag was placed in position & I clambered into it, settling in for the ride.
Once I’d mastered staying on the table, I had to have 3 dots tattooed onto my body – these are like ‘place-markers’ where the radiation beams are directed towards. I had one towards the bottom of my sternum, & one each side on each side of my ribs. They are permanent. One of my friends said that each time she sees them in the mirror, it reminds her of how grateful she is to be alive. I wholeheartedly agree with her.
Getting the right sites for the tattoos involves precision measuring with rulers, photographs & the radiotherapy machine being placed in several different positions. Co-ordinates were called out & numbers punched into the computer. I felt like a ship about to set sail.
Of course, tattoos involve needles – not great with my needle phobia & the procedure did sting because my sternum & ribs protrude. I cried when the needles went in because I’m petrified each time I’m jabbed.
The radiotherapy team had been warned in advance about my phobia, so I had one nurse tattooing me and two others looking after me. They put the radio on to distract me & the team sang a bit to the songs which was really sweet. Then we started a conversation about when you mishear lyrics & sing the wrong ones out loud, but unfortunately some of the examples that the nurses started to give (“I thought Prince was singing When Doves Die!”) made me laugh which wasn’t great for the person tattooing because she needed me to be still! However, all of this did set me up well with the team as I knew they’d be a laugh in the most daunting of situations. They reminded me to make a playlist to listen to during the procedures. Suddenly I felt a whole lot better about what lay ahead.
The radiotherapy treatment began a couple of days later. This time, a little set of steps with a handrail was put in place so I could get onto the table. It reminded me of the physio sessions at Great Ormond Street & Tadworth Hospitals – as a little kid I was obsessed with scrambling up & down the steps, so much so I’d run back to the steps when the physio put me on other equipment!
Two days into the treatment, one of the nurses piped up that they had a wheelchair hoist in the department. I laughed & said: “Well it’s too late now, I’ve taught myself how to jump on & off the table!” If I have one small wee criticism, it’s that they should have known about this hoist & offered it to me at the assessment. I did ask if there was one & told that there wasn’t one.
I clambered carefully up the steps & launched myself into the suction bag – by now, this wasn’t so comfortable, because it had set rock solid. I dutifully raised my arms into position. I hadn’t brought the right equipment to play my playlists (typically I couldn’t figure out how to connect to the hospital’s equipment because I’m a technophobe!), so some 80’s pop was playing which makes me anxious at the best of times!
A friend of a friend advised me to visualise a sunflower opening as the radiation beams were being administered. This lady had survived stage 4 cancer & was convinced that her visualisation had helped. I tried the same visualisation & as my “sunflower” was opening, I felt that I could breathe again & that the cancer was flying out of me. It was a wonderful sensation.
This experience is quite rare, but it can happen to patients; on the first & the last radiotherapy sessions, I felt the beams going in. I put it down to my particular neuropathic sensitivities & pain receptors. It felt like a burning sensation going into my ribs. I wouldn’t say that it hurt & it lasted a few moments, just very peculiar.
By the 2nd session, I’d managed to figure out how to connect my Spotify list to the hospital’s Spotify. The team allowed me to spend some time ‘being DJ’ to get it all right, so I had my bare boobs cupped in one hand & the other was setting the playlist up on their computer (oh dear, that really does sound dodgy!) I heard laughter from the team & I realised that the title of the playlist had come up on their computer at the control station – “Radiotherapy Playlist – To be played whilst my Devil’s Dumplings are being lasered”. I didn’t think the strapline would be seen, but the team loved it, explaining that their dark sense of humour was what kept them going in their profession.
Most of the radiotherapy session is taken up by the team positioning you on the table for the beams to be directed at the tattoo markers. And once you’re in position, you must keep really still which is hard when you spasm. Despite thinking that I’d chosen chilled music, I still had trouble keeping still when listening (listening to music has always been a ‘whole body’ experience for me). Plus, I’d included Hefner’s “The Greedy Ugly People” which includes these lyrics:
“Love don’t stop no wars, don’t stop no cancer…”
I honestly forgot those lyrics were in that song. Again, the radiotherapy team laughed.
The radiotherapy team were very respectful of my body & very mindful of the physical pain that I’m in due to my impairment. They never forced me into positions that I couldn’t manage (sometimes this happens when I’m having x-rays & it angers me when radiotherapists pull you into painful positions to get their image, so I was touched at how much care this team took). A couple of times I was able to get into position myself, but most of the time, I couldn’t due to the precision needed for the beams; in fact, it’s so precise that sometimes the team were moving the skin on my back & breasts by mere millimetres to get it right. When they saw that the face masks were too big for me & the corners were poking me in the eyes, they’d move the mask down. Only once did they have to interrupt the treatment to move me into a different position. I was in awe of how it all worked.
Each time, I had 3 beams. The machine moves around you & hoovers over each tattoo, & then there’s clicking noise & a beep when the laser beams into you. It felt very ‘Star Trek’. It took me a couple of sessions to get used to the movement of the machine. I wasn’t fearful, it was just disconcerting. But as soon as the beams stopped, the machine moved away, my music stopped, the room lights switched back on & the radiotherapists were helping me back off the table. Bam.
I had 5 sessions that lasted 15-20 minutes each session. At the end of the final session, my boyfriend came in & I gave him a big hug. The team gave us some time for each other. Before I left, I turned to face the table one more time, acknowledging just how physically hard that experience was for me.
Once I got outside, the team head had gathered as many of the department that he could & they gave me a huge clap. They had respect for me because they knew how hard it was for me endure those sessions. And I had respect for them for being so careful.
The team head led me towards the bell – many hospitals have this & the patient rings it when they’ve finished their treatment, or when they’re going onto their next stage. There was a brief scramble for a sanitising wipe because I insisted on cleaning the rope beforehand (COVID-19 prevention!)
I rang the bell – with a little bit of assistance from a passing patient who had the strength to ring it louder than me. Everyone cheered & clapped, including the patients in the waiting room. I’d cheered a few times for other patients; now it was my turn to get the cheers.
*Thanks to the Radiotherapy Team for giving me permission to take the photographs included in this blog*

Alt text: An edited black & white photo of me in a hospital corridor, sitting in my wheelchair, wearing a mask & ringing a large bell.